 |
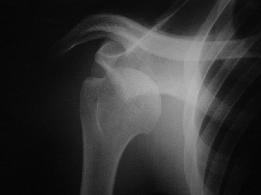
| Anteroinferior Glenohumeral Dislocation |
|
Shoulder Dislocations
A shoulder dislocation is an injury that occurs when the top of the arm bone (humerus) loses contact with the socket of the shoulder blade (scapula).
Is a shoulder dislocation the same as a shoulder separation?
No! A shoulder dislocation is often confused with a shoulder separation, but these are two very different injuries. It is important to distinguish between these two problems because the issues with management, treatment, and rehabilitation are different. If you sustained a shoulder separation rather than a shoulder dislocation, you can read more about that injury in the information on separated shoulders.
What happens when you sustain a shoulder dislocation?
The shoulder joint is made of three bones which come together at one place.
The arm bone (humerus), the shoulder blade (scapula), and the collarbone (clavicle) all meet up at the top of the shoulder. A shoulder separation shoulder separation occurs when there is an injury to the joint between the scapula and clavicle--this is called an acromioclavicular (or AC) separation. A shoulder dislocation occurs when there is an injury to the joint between the humerus and scapula.
The joint between the humerus and scapula, also called the glenohumeral joint, is a ball-and-socket joint--the ball is on the top of the humerus, and this fits into a socket of the shoulder blade called the glenoid. This joint is incredible because it allows us to move our shoulder though an amazing arc of motion--no joint in the body allows more motion than the glenohumeral joint. Unfortunately, by allowing this wide range of motion, the shoulder is not as stable as other joints. Because of this, shoulder dislocations are not uncommon injuries.
How does a shoulder dislocation happen?
A shoulder dislocation generally occurs after an injury such as a fall or a sports-related injury. About 95% of the time, when the shoulder dislocates, the top of the humerus is sitting in front of the shoulder blade--an anterior dislocation. In less than 5% of cases, the top of the humerus is behind the shoulder blade--a posterior dislocation. Posterior dislocations are unusual and seen after injuries such as electrocution or after a seizure.
What are the symptoms of a shoulder dislocation?
Patients with a shoulder dislocation are usually in significant pain. They know something is wrong, but may not know they have sustained a shoulder dislocation. Symptoms of shoulder dislocation include:
-
Shoulder pain
-
Arm held at the side, usually slightly away from the body with the forearm turned outward
-
Loss of the normal rounded contour of the deltoid muscle
How is the diagnosis of a shoulder dislocation made?
Diagnosis of a shoulder dislocation is usually quite apparent just by talking to a patient and examining their joint. Patients must be examined to determine if there is any nerve or blood vessel damage. This should be done prior to reduction (repositioning) of the shoulder dislocation. X-rays should be obtained to check for any fracture around the joint, and to determine the pattern of the shoulder dislocation. When the shoulder dislocation is diagnosed, the shoulder must be "reduced," or put back in place.
Should a shoulder dislocation be reduced "in the field" or in the ER?
It is possible to treat a shoulder dislocation at the scene of the injury, but if transportation to a hospital is available, then this is a much safer option. If a trained provider is available, then a shoulder dislocation can often be easily reduced soon after the injury. In this period of time immediately following the injury, the muscles are not yet in spasm, and the shoulder dislocation can usually be reduced with some basic maneuvers.
However, there are potential complications of a shoulder dislocation, and there are possible complications of reducing a dislocated shoulder. Therefore, if trained personnel are not available, or if there are signs of unusual circumstances, reduction of the shoulder dislocation is best done in trained hands at a hospital.
How is a shoulder dislocation reduced?
There are several methods to reduce the shoulder dislocation into its normal position. If the patient is in the emergency room, the patient will receive anesthesia for the procedure. The two most commonly used types of anesthesia include:
Intravenous (IV) Sedation
Most commonly, patients with a shoulder dislocation are given IV anesthesia. This both alleviates pain, and makes the patient unconscious for a few minutes. During that time, the physician can manipulate the shoulder dislocation back into position.
Local Injection
Injection of Novocaine into the joint can provide ample anesthesia to perform a reduction of a shoulder dislocation. Recent studies have shown this type of anesthesia to be just as effective as IV anesthesia, but these patients tend to leave the ER more quickly because they do not have to allow time for the anesthesia to wear off.
There are several maneuvers that can be used to reposition a shoulder dislocation--usually each physician has a favored reduction maneuver. In general, the goal is to manipulate the bones to allow them to slide back into position without causing further damage to the shoulder joint.
Once the should dislocation is back in place, repeat x-rays are performed to ensure it is indeed in the correct position, and to evaluate for other injuries such as fractures. Patients are placed in a sling to rest the shoulder and referred to their orthopedic surgeon for further management.
Is further treatment needed for a shoulder dislocation?
Patients who sustain a shoulder dislocation are much more likely to have another shoulder dislocation. The reason is that when a shoulder dislocation occurs, ligaments within the shoulder are torn and the shoulder joint becomes less stable.
Most often a patient will be examined by their orthopaedic surgeon. If a shoulder dislocation occurred, the examiner will look for signs of injury to the ligaments in the shoulder--most often the so-called Bankart lesion. This may include some specific tests to evaluate for shoulder instability. A MRI test may be obtained to look for the Bankart lesion. If ligament damage is diagnosed, a decision about whether or not to proceed with surgical treatment must be made.
Can shoulder dislocations be treated without surgery?
Surgical treatment of a shoulder dislocation is most often recommended for patients who have recurrent, or repeat, shoulder dislocations. In some patients, surgery may be recommended after a first shoulder dislocation.
The problem with non-surgical treatment of shoulder dislocations is that the normal ligament “bumper” that keeps the shoulder from dislocating is torn away from the glenoid.
Most shoulder dislocations are anterior shoulder dislocations, meaning the ball is pushed out it front of the socket. About 95% of shoulder dislocations are anterior. In patients who sustain this type of shoulder dislocation, the most common injury in the shoulder is called a Bankart lesion. Bankart lesion. The "Bankart lesion" means that ligaments that help to hold the shoulder in proper position have been damaged.
The Bankart lesion occurs in over 90% of patients with an anterior shoulder dislocation. When the ligament is torn in patients with this Bankart lesion, the shoulder is not held as tightly in position.
Can the Bankart lesion heal without surgery?
Yes. In fact, it will always heal. The problem is that it does not heal in the right position. The ligament tends to heal in a position that does not help to hold the shoulder in the proper position.
What are the results with surgery?
With modern arthroscopic techniques, the redislocation rate in published studies is 8%. The majority of those that redislocate tend to be contact athletes (e,g, football, hockey).
How is the surgery accomplished?
Surgery is performed on an outpatient basis and generally takes 1 to 2 hours. The torn ligaments and labrum are reattached back to the glenoid using sutures attached to anchors that are placed in the glenoid. The anchors used are made of a special plastic that the body reabsorbs after 12 to 18 months but the sutures are permanent. If the ligaments are tied down to freshened bone, the body will send special tissues called Sharpey’s fibers to permanent heal the ligament to the bone. It takes approximately 12 weeks for ligaments to heal.
Usual Nonoperative Treatment of Shoulder Dislocations
The usual treatment of an anterior shoulder dislocation is to place the patient in a sling for a few weeks to allow the swelling and inflammation around the shoulder to subside. Thereafter, progressive exercises are started until the patient is able to resume their usual activities.
The sling that is used to treat most shoulder dislocations holds the shoulder in internal rotation. This means that the shoulder is turned inwards, and the forearm is held against the body. When the shoulder is held in internal rotation the ligament that is torn (the Bankart lesion) is often held in a non-anatomic position. When it heals, it tends to heal in an improper position. In some patients, especially younger patients, healing of the ligament in this position may lead to repeat shoulder dislocations.
Immobilization of Shoulder Dislocations in External Rotation
Research out of Japan has shed light on the treatment of shoulder dislocations with the shoulder held in external rotation. When the shoulder is held in external rotation the ligament is brought into a more normal position, and may heal in this proper position. The idea behind immobilization in external rotation is that if the ligament heals in the proper position, then repeat shoulder dislocations will be less likely.
Immobilization in external rotation of shoulder dislocations may be appropriate for some people. It is important that the external rotation brace be properly configured--the arm should be held tightly against the side, and the forearm should be pointing away from the body. Many patients (and some doctors) confuse abduction immobilizers (shoulder immobilizers with a pillow in the armpit) with an external rotation immobilizer. These are not the same, and similar results of treatment should not be expected. (Reference: Itoi, E, et al. "A new method of immobilization after traumatic anterior dislocation of the shoulder: a preliminary study." J Shoulder Elbow Surg. 2003 Sep-Oct;12(5):413-5)
Does a brace help to prevent shoulder dislocation?
Bracing is sometimes considered for patients who sustain a shoulder dislocation. A brace is most commonly used for an in-season athlete who sustains a shoulder dislocation. In this scenario, surgery for treatment of the shoulder dislocation would be season-ending. Therefore, a brace may be used to help prevent a shoulder dislocation.
Are braces effective at preventing shoulder dislocations?
The braces can help to prevent the shoulder from being placed into a position in which a dislocation is possible. While they cannot prevent all shoulder dislocations, these braces can reduce the overall incidence of shoulder dislocations in athletes.
Can the braces be worn during competition?
This is the real problem, and why bracing plays a very small role in the treatment and prevention of shoulder dislocations.
Athletes who participate in sports often have difficulty wearing the brace and competing effectively. Braces are especially cumbersome in athletes who overhead function (such as throwing) is critical for their effectiveness. Therefore, most athletes are unable to return to their sport while wearing a shoulder dislocation brace.
* Portions borrowed with permission from Jonathan Cluett, M.D., More information can be found at http://orthopedics.about.com .
Dr. Cluett was a SMOG Fellow from 2005 – 2006.
|